
Michelle Klaiman
Emergency Physician and Addictions Specialist
My biggest fear is that my patients are going to die. I fear this on a daily basis.
The pandemic has been difficult on us all, but imagine someone with opiate-use disorder who has lost all their community addictions or mental health support, who has lost their sense of community because everyone is trying to self-isolate, and no longer has access to the same resources. That isolation combined with feelings of anxiety or depression can lead to increased use.
We’ve seen a 25 per cent increase in opiate-related overdose deaths in a three month period, compared with the same three months last year. It’s been devastating for the community.
We know that if someone is started on treatment immediately, their chances of staying on treatment is much higher. If we tell someone to come back three days later for a clinic appointment, the chances of them showing up is less than 30 per cent.
It’s very upsetting to discharge a patient or to watch them leave against medical advice before they’ve received treatment. It makes me feel sad. Actually, sad feels like too simple of a word.
It makes me think, “I should have pushed it a little more,” or “I could have done better.”
I pray that they don’t overdose before they come back. I’ve seen that happen with my patients before. It’s so defeating. It makes me think, “I should have pushed it a little more,” or “I could have done better.” I try to remember the successes when that happens. I think about the pregnant patient who got on treatment to avoid apprehension of her child by Children’s Aid. I remind myself that a brief intervention can lead to meaningful change.
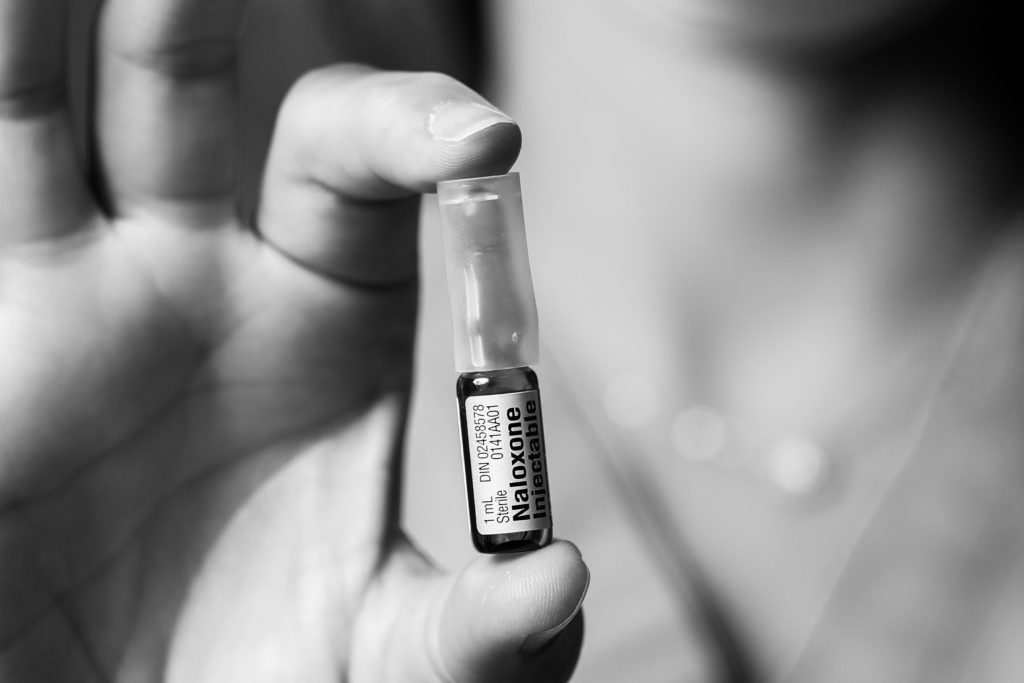
I’ve had patients in my community practice who I think are stable. They were back at work and doing quite well, on methadone, then they relapsed. Now that the drug supply is so toxic and potent with fentanyl and carfentanil, they’ve lost their tolerance and they can die with single use especially if they use alone. That’s really what keeps me up at night.
My patients look at me and they might think I can’t relate to them. “You’re a successful physician, you have a family – three kids, a husband, a house, a car, a good life.” But I’ve been through my own adversities and I’ve had to be resilient in my own way.
I went through a lot when I had my twins, they were very early, and when I was pregnant with them my father passed away and he suffered from depression himself.
It might not be the same as somebody sleeping rough on the street who is injecting crystal meth every day just to survive. But I can understand on some level what my patients are going through.
I understand hardships. I understand resiliency.
Dr. Michelle Klaiman is an emergency physician and addictions specialist at St. Michael’s Hospital.
As told to Jennifer Stranges. Photos by Katie Cooper. This interview has been edited and condensed.

